Who could have predicted at the start of 2020 what a turmoil the COVID pandemic would throw us into? It really is unprecedented when the Government tells you to stop what you are doing, send your staff home and close your door!

When this happened on March 25th, our diary was full of patient appointments, with 3; 6; 9 and 12 monthly recalls, booked right the way through to 2021. All this went by the wayside like so many other well-laid plans and through implementing all the best practice, professional guidelines in order to safely re-open in June, it became evident that the rest of 2020 would be taken up with only seeing a fraction of our database of patients, those who needed urgent dental care!
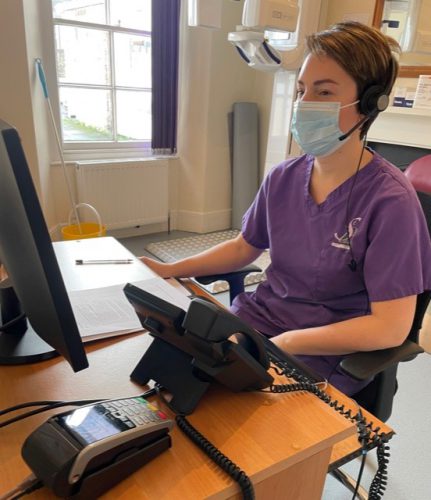
It was extremely frustrating and demoralising for our Dentists not to be able to see anyone during the first Lockdown and have limited resources to deal with patients’ problems but I’m sure it was reassuring to you all, that there was at least a familiar voice on the end of the phone, as they shared amongst themselves the ‘on call’ responsibility each week.
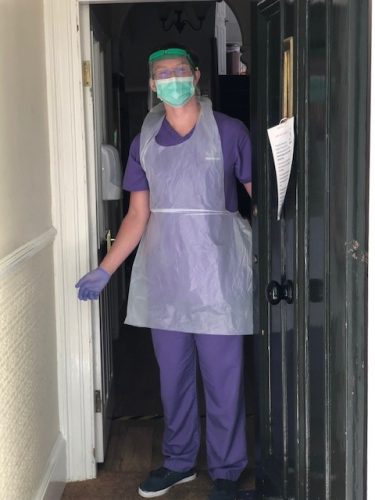
For Nick, this wasn’t enough and he very quickly volunteered to assist at the Urgent Dental Care Hub in Torquay, about the only place at the time able to see patients face to face.
It is worth considering some additions to your first aid kit, should you find yourself without access to a Dentist again, maybe if travelling or working away for any length of time. Most items are available from chemists, supermarkets or online and like most things nowadays, you can even access great YouTube videos of how to apply them.
-
- Temporary filling material. If you lose a filling, you want to plug the hole quickly. It’s a paste-like material that fills the hole and helps provide relief from sensitivity and harmful bacteria.
- Dental wax. A soft material that can be used to temporarily cover sharp surfaces inside your mouth, such as broken teeth, orthodontic wires. (The wax surrounding cheese can also be useful)
- Vaseline. To temporarily attach a crown, it’s easier to clean off than adhesives. Just fill the crown, pop it on, and the gel makes a seal that holds it temporarily in place.
- Floss: Food stuck between teeth can definitely cause a great deal of pain and damage.
- Nail file. Can be used to smooth over the sharp edge of a broken tooth and save your tongue, cheeks from damage and ulcers.
During the first Lockdown we dealt with 350 people in trouble and as soon as we were allowed to re-open we got to work, booking appointments for these people and catching up with all the others whose treatment had been put on hold due to COVID.
The way we operate has completely changed, with additional measures in place to keep everyone safe here at St. Paul’s, details of which can be found under ‘The patient journey during COVID 19’ https://www.stpaulsdentalpractice.co.uk/routine-appointments.html
With so many restrictions in place, we have worked hard to get as many people through the door as possible since June. We have prioritised those with urgent treatment needs and those who are at risk of deteriorating oral health if not seen, covering all age ranges.

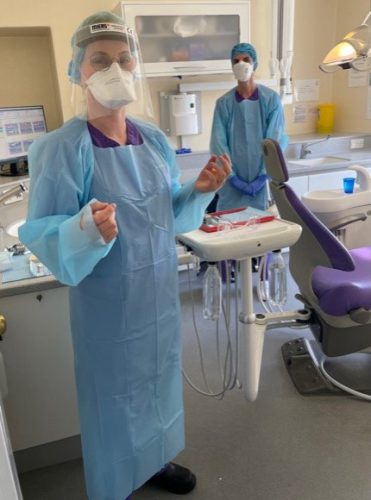
Our team has worked without a single moan or winge, despite additional working pressure, the constraints of wearing additional PPE, tighter regulations to follow and all without the usual rewards of social gatherings, team building days or even just all being able to sit down together and relax.
We were grateful to have the added support of Nichola, who joined our team in June this year and we are yet to see what she really looks like behind the mask.
Despite our best efforts, since re-opening we have only managed to see about 25% of all our patients! We are fully aware how many of you have missed out on your routine appointments and we hope with the news of vaccinations becoming available, there will be some point in the not too distant future that we will be able to open all our surgeries and recommence normal appointments.
Meanwhile, we will continue to keep in touch as best we can, by newsletters, social media, texts, emails and through our website.
In addition, Anna one of our Oral Health Educators has created some videos of oral health care advice which you can find on YouTube https://www.youtube.com/c/StpaulsdentalpracticeUk/videos
If you want to hear from us, keep your contact details up to date and inform us if there are any changes.
Contact us by email info@stpaulsdentalpractice.co.uk; our webform or phone 01626 365896. We are here to answer any dental concerns you have and see you when necessary.
Remember now more than ever how important your daily oral care routine is as well as checking regularly for any changes in your mouth, being vigilant for signs of mouth cancer. https://www.dentalhealth.org/
Don’t forget, we stock a good range of all the Dental Care Products you will need for your home routine and these can be paid for by phone and posted out to you, without the need to leave your home.
Our Christmas opening times are listed on our website and a recorded message will be available on our phones, with details of when we are there or when to call the ‘out of hours’ service. https://www.stpaulsdentalpractice.co.uk/find-dentists-devon.html
We very much look forward to seeing you in 2021 and would like to wish all our valued patients a very Merry Christmas and a Happy New Year.

http://www.freepik.com





 Photo courtesy of freerangestock.com/photographer/Candace-McDaniel
Photo courtesy of freerangestock.com/photographer/Candace-McDaniel